Abstract
Background
Systemic AA amyloidosis is a recognised complication of inflammatory bowel disease. AA amyloidosis is a potential cause of end-stage renal failure and mortality but little is known of the natural history of this condition in inflammatory bowel disease.
Methods
We evaluated the clinical phenotype, disease progression and outcome amongst 26 patients with inflammatory bowel disease and AA amyloidosis followed prospectively at a single center between 1989 and 2010.
Results
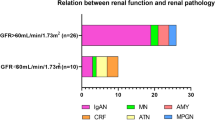
Twenty-two patients had Crohn’s disease and four had ulcerative colitis. Fistulae and abscesses occurred in ten cases, all of whom had Crohn’s disease. Amyloidotic proteinuric renal dysfunction occurred in all of the cases. It resolved in five patients with well-controlled inflammation, but was progressive in all of the other patients. Fifteen patients reached end-stage renal disease after a median time of 6.3 years from development of renal dysfunction (by Kaplan–Meier estimate), six of whom subsequently proceeded to renal transplantation. There were five functioning grafts at census 0.8, 3.2, 4.2, 20.1 and 24.6 years after transplantation. One graft failed 14.5 years after renal transplantation because of amyloid recurrence in a patient with sustained chronic inflammatory activity.
Conclusions
AA amyloidosis remains a serious complication of both Crohn’s disease and ulcerative colitis, and is characterized by proteinuric renal dysfunction that may resolve following suppression of inflammatory activity. Patient and graft survival are excellent in patients who undergo renal transplantation.


Similar content being viewed by others
References
Hawkins PN. Systemic amyloidosis. In: Weinsten WM, Hawkey CJ, Bosch J, eds. Clinical Gastroenterolgy and Hepatology. City: Elsevier Health Sciences; 2005:853–858.
Alishiri GH, Salimzadeh A, Owlia MB, Forghanizadeh J, Setarehshenas R, Shayanfar N. Prevalence of amyloid deposition in long standing rheumatoid arthritis in Iranian patients by abdominal subcutaneous fat biopsy and assessment of clinical and laboratory characteristics. BMC Musculoskelet Disord. 2006;7:43.
Koivuniemi R, Paimela L, Suomalainen R, Tornroth T, Leirisalo-Repo M. Amyloidosis is frequently undetected in patients with rheumatoid arthritis. Amyloid. 2008;15:262–268.
Lachmann HJ, Goodman HJB, Gilbertson JA, et al. Natural history and outcome in systemic AA amyloidosis. N Engl J Med. 2007;356:2361–2371.
Urieli-Shoval S, Linke RP, Matzner Y. Expression and function of serum amyloid A, a major acute-phase protein, in normal and disease states. Curr Opin Hematol. 2000;7:64–69.
Lachmann HJ, Booth DR, Booth SE, et al. Misdiagnosis of hereditary amyloidosis as AL (primary) amyloidosis. N Engl J Med. 2002;346:1786–1791.
Lachmann HJ, Gallimore R, Gillmore JD, et al. Outcome in systemic AL amyloidosis in relation to changes in concentration of circulating free immunoglobulin light chains following chemotherapy. Br J Haematol. 2003;122:78–84.
Puchtler H, Sweat F, Levine M. On the binding of Congo red by amyloid. J Histochem Cytochem. 1962;10:355–364.
Hawkins PN, Lavender JP, Pepys MB. Evaluation of systemic amyloidosis by scintigraphy with 123I-labeled serum amyloid P component. N Engl J Med. 1990;323:508–513.
Poole S, Walker D, Gaines Das RE, Gallimore JR, Pepys MB. The first international standard for serum amyloid A protein (SAA). Evaluation in an international collaborative study. J Immunol Methods. 1998;214:1–10.
Moschkowitz E. The clinical aspects of amyloidosis. Ann Intern Med. 1936;10:73–89.
Werther JL, Schapira A, Rubinstein O, Janowitz HD. Amyloidosis in regional enteritis. A report of five cases. Am J Med. 1960;29:416–423.
Mir-Madjlessi SH, Brown CH, Hawk WA. Amyloidosis associated with Crohn’s disease. Am J Gastroenterol. 1972;58:563–577.
Lovat LB, Madhoo S, Pepys MB, Hawkins PN. Long term survival in systemic AA amyloidosis complicating Crohn’s disease. Gastroenterology. 1997;112:1362–1365.
Greenstein AJ, Sachar DB, Panday AK, et al. Amyloidosis and inflammatory bowel disease. A 50-year experience with 25 patients. Medicine (Baltimore). 1992;71:261–270.
Wester AL, Vatn MH, Fausa O. Secondary amyloidosis in inflammatory bowel disease: a study of 18 patients admitted to Rikshospitalet University Hospital, Oslo, from 1962 to 1998. Inflamm Bowel Dis. 2001;7:295–300.
Weterman IT, Biemond I, Pena AS. Mortality and causes of death in Crohn’s disease. Review of 50 years’ experience in Leiden University Hospital. Gut. 1990;31:1387–1390.
Saverymuttu SH, Hodgson HJF, Chadwick VS, Pepys MB. Differing acute phase responses in Crohn’s disease and ulcerative colitis. Gut. 1986;27:809–813.
Immonen K, Finne P, Hakala M, Kautiainen H, Pettersson T, Gronhagen-Riska C. No improvement in survival of patients with amyloidosis associated with inflammatory rheumatic diseases—data from the Finnish national registry for kidney diseases. J Rheumatol. 2008;35:1334–1338.
Izzedine H, Simon J, Piette AM, et al. Primary chronic interstitial nephritis in Crohn’s disease. Gastroenterology. 2002;123:1436–1440.
Van Rooijen N, Sanders A. Liposome mediated depletion of macrophages: mechanism of action, preparation of liposomes and applications. J Immunol Methods. 1994;174:83–93.
Gillmore JD, Lovat LB, Persey MR, Pepys MB, Hawkins PN. Amyloid load and clinical outcome in AA amyloidosis in relation to circulating concentration of serum amyloid A protein. Lancet. 2001;358:24–29.
Ramadas AV, Gunesh S, Thomas GA, Williams GT, Hawthorne AB. Natural history of Crohn’s disease in a population-based cohort from Cardiff (1986–2003): a study of changes in medical treatment and surgical resection rates. Gut. 2010;59:1200–1206.
Iizuka M, Sagara S, Etou T. Efficacy of scheduled infliximab maintenance therapy on systemic amyloidosis associated with Crohn’s disease. Inflamm Bowel Dis. 2011;17:E67–E68.
Fernandez-Nebro A, Urena I, Irigoyen MV, Garcia-Vicuna R. Anti-TNF-alpha for treatment of amyloidosis associated with Crohn’s disease. Gut. 2006;55:1666–1667.
Akobeng AK. Review article: the evidence base for interventions used to maintain remission in Crohn’s disease. Aliment Pharmacol Ther. 2008;27:11–18.
Lachmann HJ, Gillmore JD, Wechalekar AD, et al. Survival on dialysis and outcome after renal transplantation in AA amyloidosis. Amyloid. 2010;17(Suppl. 1):73.
Ozdemir BH, Ozdemir FN, Sezer S, Sar A, Haberal M. Among therapy modalities of end-stage renal disease, renal transplantation improves survival in patients with amyloidosis. Transplant Proc. 2006;38:432–434.
Acknowledgments
We thank our many colleagues for referring and caring for the patients: T. Lane, A. Hughes, E. Pyart, D. Gopaul and D. Hutt for their technical and clinical support at the National Amyloidosis Centre. We thank J. Berkeley for expert preparation of the manuscript.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sattianayagam, P.T., Gillmore, J.D., Pinney, J.H. et al. Inflammatory Bowel Disease and Systemic AA Amyloidosis. Dig Dis Sci 58, 1689–1697 (2013). https://doi.org/10.1007/s10620-012-2549-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-012-2549-x