Abstract
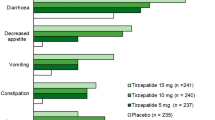
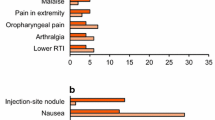
Pramlintide, the first member of a new class of drugs for the treatment of insulin-using patients with type 2 or type 1 diabetes mellitus, is an analog of the peptide hormone amylin. Amylin is co-secreted with insulin from pancreatic β cells and acts centrally to slow gastric emptying, suppress postprandial glucagon secretion, and decrease food intake. These actions complement those of insulin to regulate blood glucose concentrations. Amylin is relatively deficient in patients with type 2 diabetes, depending on the severity of β-cell secretory failure, and is essentially absent in patients with type 1 diabetes. Through mechanisms similar to those of amylin, pramlintide improves overall glycemic control, reduces postprandial glucose levels, and reduces bodyweight in patients with diabetes using mealtime insulin. Reductions in postprandial glucose and bodyweight are important, since postprandial hyperglycemia is associated with an increased risk of microvascular and macrovascular complications, and increased weight is an independent risk factor for cardiovascular disease. Pramlintide is generally well tolerated, with the most frequent treatment-emergent adverse event being mild to moderate nausea, which decreases over time. Pramlintide treatment is also associated with improvements in markers of oxidative stress and cardiovascular risk and improved patient-reported treatment satisfaction. These factors make pramlintide an attractive option for the treatment of postprandial hyperglycemia in patients with diabetes using mealtime insulin.











Similar content being viewed by others
References
International Diabetes Federation. Did you know? [online]. Available from URL: http://www.idf.org/home/index.cfm?node=37 [Accessed 2008 Jun 11]
American Diabetes Association. Standards of medical care in diabetes: 2008. Diabetes Care 2008; 31Suppl. 1: S12–54
Edelman SV, Weyer C. Unresolved challenges with insulin therapy in type 1 and type 2 diabetes: potential benefit of replacing amylin, a second β-cell hormone. Diabetes Technol Ther 2002; 4(2): 175–89
The Diabetes Control and Complications Trial Research Group. The effect of intensive treatment of diabetes on the development and progression of long-term complications in insulin-dependent diabetes mellitus. N Engl J Med 1993; 329(14): 977–86
UK Prospective Diabetes Study (UKPDS) Group. Intensive blood-glucose control with sulphonylureas or insulin compared with conventional treatment and risk of complications in patients with type 2 diabetes (UKPDS 33). Lancet 1998; 352(9131): 837–53
Nichols GA, Gomez-Caminero A. Weight changes following the initiation of new anti-hyperglycaemic therapies. Diabetes Obes Metab 2007 Jan; 9(1): 96–102
Purnell J, Weyer C. Weight effect of current and experimental drugs for diabetes mellitus: from promotion to alleviation of obesity. Treat Endocrinol 2003; 2(1): 33–47
Holman RR, Thorne KI, Farmer AJ, et al. Addition of biphasic, prandial, or basal insulin to oral therapy in type 2 diabetes. N Engl J Med 2007; 357(17): 1716–30
Zammitt NN, Frier BM. Hypoglycemia in type 2 diabetes: pathophysiology, frequency, and effects of different treatment modalities. Diabetes Care 2005 Dec; 28(12): 2948–61
Buse JB, Ginsbert HN, Bakris GL, et al. Primary prevention of cardiovascular diseases in people with diabetes mellitus: a scientific statement from the American Heart Association and the American Diabetes Association. Diabetes Care 2007 Jan; 30(1): 162–72
Young AA, Gedulin B, Vine W, et al. Gastric emptying is accelerated in diabetic BB rats and is slowed by subcutaneous injections of amylin. Diabetologia 1995; 38(6): 642–8
Gedulin B, Percy A, Jodka C, et al. Studies using neutralizing antibody and the antagonist AC187 reveal that endogenous amylin inhibits glucagon secretion [abstract no. 1179]. Diabetologia 1997; 40Suppl. 1: A300
Bhavsar S, Watkins J, Young A. Synergy between amylin and cholecystokinin for inhibition of food intake in mice. Physiol Behav 1998; 64(4): 557–61
Kruger DF, Gatcomb PM, Owen SK. Clinical implications of amylin and amylin deficiency. Diabetes Educ 1999; 25(3): 389–97; quiz 398
Nowak TV, Johnson CP, Wood CM, et al. Evidence for accelerated gastric emptying in asymptomatic patients with insulin-dependent diabetes mellitus [abstract]. Gastroenterology 1990; 98(5 Pt 2): A378
Phillips WT, Schwartz JG, McMahan CA. Rapid gastric emptying of an oral glucose solution in type 2 diabetic patients. J Nucl Med 1992; 33(8): 1496–500
Maggs D, MacDonald I, Nauck MA. Glucose homeostasis and the gastrointestinal tract: insights into the treatment of diabetes. Diabetes Obes Metab 2008; 10(1): 18–33
Schvarcz E, Palmer M, Aman J, et al. Physiological hyperglycemia slows gastric emptying in normal subjects and patients with insulin-dependent diabetes mellitus. Gastroenterology 1997; 113(1): 60–6
Bertin E, Schneider N, Abdelli N, et al. Gastric emptying is accelerated in obese type 2 diabetic patients without autonomic neuropathy. Diabetes Metab 2001 Jun; 27(3): 357–64
Gedulin BR, Young AA. Hypoglycemia overrides amylin-mediated regulation of gastric emptying in rats. Diabetes 1998; 47(1): 93–7
Unger RH, Orci L. The role of glucagon in the endogenous hyperglycemia of diabetes mellitus. Annu Rev Med 1977; 28: 119–30
Silvestre RA, Rodriguez-Gallardo J, Jodka C, et al. Selective amylin inhibition of the glucagon response to arginine is extrinsic to the pancreas. Am J Physiol Endocrinol Metab 2001; 280(3): E443–9
Reidelberger RD, Arnelo U, Granqvist L, et al. Comparative effects of amylin and cholecystokinin on food intake and gastric emptying in rats. Am J Physiol Regul Integr Comp Physiol 2001; 280(3): R605–11
Granqvist L, Permert J, Arnelo U, et al. Effects of AC187, IAPP(8–37) and CGRP(8-37) on IAPP induced anorexia in rats [abstract no. 218]. Digestion 1997; 58Suppl. 2: 55
Reidelberger RD, Haver AC, Arnelo U, et al. Amylin receptor blockade stimulates food intake in rats. Am J Physiol Regul Integr Comp Physiol 2004 Sep; 287(3): R568–74
Amylin Pharmaceuticals Inc. Symlin™ (pramlintide acetate) injection [package insert]. San Diego (CA): Amylin Pharmaceuticals Inc., 2008 [online]. Available from URL: http://www.symlin.com/pdf/SYMLIN-pi-combined.pdf [Accessed 2008 Oct 28]
Maggs DG, Fineman M, Kornstein J, et al. Pramlintide reduces postprandial glucose excursions when added to insulin lispro in subjects with type 2 diabetes: a dose timing study. Diabetes Metab Res Rev 2004 Jan-Feb 28; 20(1): 55–60
Weyer C, Gottlieb A, Kim DD, et al. Pramlintide reduces postprandial glucose excursions when added to regular insulin or insulin lispro in subjects with type 1 diabetes: a dose-timing study. Diabetes Care 2003 Nov; 26(11): 3074–9
Edelman SV, Schroeder BE, Frias JP. Pramlintide acetate in the treatment of type 2 and type 1 diabetes mellitus. Exp Rev Endocrinol Metab 2007; 2: 9–18
Samsom M, Szarka LA, Camilleri M, et al. Pramlintide, an amylin analog, selectively delays gastric emptying: potential role of vagal inhibition. Am J Physiol 2000; 278(6): G946–51
Vella A, Lee JS, Camilleri M, et al. Effects of pramlintide, an amylin analogue, on gastric emptying in type 1 and 2 diabetes mellitus. Neurogastroenterol Motil 2002 Apr; 14(2): 123–31
Fineman MS, Koda JE, Shen LZ, et al. The human amylin analog, pramlintide, corrects postprandial hyperglucagonemia in patients with type 1 diabetes. Metabolism 2002; 51(5): 636–41
Chapman I, Parker B, Doran S, et al. Effect of pramlintide on satiety and food intake in obese subjects and subjects with type 2 diabetes. Diabetologia 2005 May; 48(5): 838–48
Fineman M, Weyer C, Maggs DG, et al. The human amylin analog, pramlintide, reduces postprandial hyperglucagonemia in patients with type 2 diabetes mellitus. Horm Metab Res 2002 Sep; 34(9): 504–8
Nyholm B, Orskov L, Hove K, et al. The amylin analog pramlintide improves glycemic control and reduces postprandial glucagon concentrations in patients with type 1 diabetes mellitus. Metabolism 1999; 48(7): 935–41
UK Prospective Diabetes Study Group. UK Prospective Diabetes Study 16. Overview of 6 years’ therapy of type II diabetes: a progressive disease [published erratum appears in Diabetes 1996 Nov; 45(11): 1655]. Diabetes 1995 Nov; 44 (11): 1249–58
DeFronzo RA. Pharmacologic therapy for type 2 diabetes mellitus. Ann Intern Med 1999; 131 (4): 281–303
Hepburn DA, MacLeod KM, Pell AC, et al. Frequency and symptoms of hypogly-caemia experienced by patients with type 2 diabetes treated with insulin. Diabet Med 1993 Apr; 10(3): 231–7
Henry RR, Gumbiner B, Ditzler T, et al. Intensive conventional insulin therapy for type II diabetes: metabolic effects during a 6-mo outpatient trial. Diabetes Care 1993 Jan; 16(1): 21–31
Gurlek A, Erbas T, Gedik O. Frequency of severe hypoglycaemia in type 1 and type 2 diabetes during conventional insulin therapy. Exp Clin Endocrinol Diabetes 1999; 107(3): 220–4
Hollander PA, Levy P, Fineman MS, et al. Pramlintide as an adjunct to insulin therapy improves long-term glycemie and weight control in patients with type 2 diabetes: a 1-year randomized controlled trial. Diabetes Care 2003 Mar; 26(3): 784–90
Gottlieb A, Fineman M, Bahner A, et al. Pramlintide therapy in addition to insulin in type 2 diabetes: effect on metabolic control after 6 months [abstract no. 0873]. Diabetologia 1999; 42Suppl. 1: A232
Ratner RE, Want LL, Fineman MS, et al. Adjunctive therapy with the amylin analogue pramlintide leads to a combined improvement in glycemie and weight control in insulin-treated subjects with type 2 diabetes. Diabetes Technol Ther 2002; 4(1): 51–61
Whitehouse F, Kruger DF, Fineman M, et al. A randomized study and open-label extension evaluating the long-term efficacy of pramlintide as an adjunct to insulin therapy in type 1 diabetes. Diabetes Care 2002; 25(4): 724–30
Ratner RE, Dickey R, Fineman M, et al. Amylin replacement with pramlintide as an adjunct to insulin therapy improves long-term glycaemic and weight control in type 1 diabetes mellitus: a 1-year randomized controlled trial. Diabet Med 2004 Nov; 21 (11): 1204–12
Fineman M, Gottlieb A, Bahner A, et al. Pramlintide therapy in addition to insulin in type 1 diabetes: effect on metabolic control after 6 months [abstract no. 0872]. Diabetologia 1999; 42Suppl. 1: A232
Guthrie R, Karl D, Wang Y, et al. In an open-label clinical study pramlintide lowered A1C, body weight, and insulin use in patients with type 1 diabetes failing to achieve glycemic targets with insulin therapy [abstract no. 478-P]. Diabetes 2005 Jun; 54Suppl. 1: A118
Karl D, Philis-Tsimikas A, Darsow T, et al. Pramlintide as an adjunct to insulin in patients with type 2 diabetes in a clinical practice setting reduced A1C, postprandial glucose excursions and weight. Diabetes Technol Ther 2007 Apr; 9(2): 191–9
Pullman J, Darsow T, Frias JP. Pramlintide in the management of insulin-using patients with type 2 and type 1 diabetes. Vasc Health Risk Manag 2006; 2(3): 203–12
Riddle M, Frias J, Zhang B, et al. Pramlintide improved glycemic control and reduced weight in patients with type 2 diabetes using basal insulin. Diabetes Care 2007 Nov; 30(11): 2794–9
Edelman S, Garg S, Frias J, et al. A double-blind, placebo-controlled trial assessing pramlintide treatment in the setting of intensive insulin therapy in type 1 diabetes. Diabetes Care 2006 Oct; 29(10): 2189–95
Ceriello A, Hanefeld M, Leiter L, et al. Postprandial glucose regulation and diabetic complications. Arch Intern Med 2004 Oct 25; 164(19): 2090–5
Brownlee M. Biochemistry and molecular cell biology of diabetic complications. Nature 2001 Dec 13; 414(6865): 813–20
Monnier L, Mas E, Ginet C, et al. Activation of oxidative stress by acute glucose fluctuations compared with sustained chronic hyperglycemia in patients with type 2 diabetes. JAMA 2006 Apr 12; 295(14): 1681–7
Ceriello A, Lush CW, Darsow T, et al. Pramlintide reduced markers of oxidative stress in the postprandial period in patients with type 2 diabetes. Diabetes Metab Res Rev 2008 Feb; 24(2): 103–8
Ceriello A, Piconi L, Quagliaro L, et al. Effects of pramlintide on postprandial glucose excursions and measures of oxidative stress in patients with type 1 diabetes. Diabetes Care 2005 Mar; 28(3): 632–7
Purnell JQ, Hokanson JE, Marcovina SM, et al. Effect of excessive weight gain with intensive therapy of type 1 diabetes on lipid levels and blood pressure: results from the DCCT. Diabetes Control and Complications Trial. JAMA 1998; 280(2): 140–6
Pearson TA, Mensah GA, Alexander RW, et al. Markers of inflammation and cardiovascular disease: application to clinical and public health practice. A statement for healthcare professionals from the Centers for Disease Control and Prevention and the American Heart Association. Circulation 2003 Jan 28; 107(3): 499–511
Lush C, Frias J, Zhang B, et al. Pramlintide, as an adjunct to basal insulin, reduced C-reactive protein, improved glycemic control, and led to weight loss in patients with type 2 diabetes [abstract no. 541-P]. Diabetes 2007 Jun; 56Suppl. 1: A144
Lush C, Frias J, Nanayakkara N, et al. Effect of adjunctive pramlintide treatment on hsCRP and adiponectin levels in intensively treated patients with type 1 diabetes [abstract no. 0254]. Diabetologia 2006 Sep; 49Suppl. 1: 160–1
Costacou T, Zgibor JC, Evans RW, et al. The prospective association between adiponectin and coronary artery disease among individuals with type 1 diabetes. The Pittsburgh Epidemiology of Diabetes Complications Study. Diabetologia 2005 Jan; 48(1): 41–8
Maahs DM, Ogden LG, Kinney GL, et al. Low plasma adiponectin levels predict progression of coronary artery calcification. Circulation 2005 Feb 15; 111(6): 747–53
Marrero DG, Crean J, Zhang B, et al. Effect of adjunctive pramlintide treatment on treatment satisfaction in patients with type 1 diabetes. Diabetes Care 2007 Feb; 30(2): 210–6
Rubin RR, Peyrot M. Assessing treatment satisfaction in patients treated with pramlintide as an adjunct to insulin therapy. Curr Med Res Opin 2007; 23(8): 1919–29
Jodka C, Green D, Young A, et al. Amylin modulation of gastric emptying in rats depends upon an intact vagus nerve [abstract no. 867]. Diabetes 1996; 45Suppl. 2: 235A
Lutz TA, Mollet A, Rushing PA, et al. The anorectic effect of a chronic peripheral infusion of amylin is abolished in area postrema/nucleus of the solitary tract (AP/NTS) lesioned rats. Int J Obes Relat Metab Disord 2001; 25(7): 1005–11
Mack C, Hoyt J, Moore C, et al. Sustained reduction in food intake and body weight in high fat-fed rats during 28-day amylin infusion [abstract no. 1690-P]. Diabetes 2003 Jun; 52Suppl. 1: A389
Rushing PA. Central amylin signaling and the regulation of energy homeostasis. Curr Pharm Des 2003; 9(10): 819–25
Rushing PA, Hagan MM, Seeley RJ, et al. Inhibition of central amylin signaling increases food intake and body adiposity in rats. Endocrinology 2001; 142(11): 5035–8
Smith SR, Blundell JE, Burns C, et al. Pramlintide treatment reduces 24-h caloric intake and meal sizes and improves control of eating in obese subjects: a 6-wk translational research study. Am J Physiol Endocrinol Metab 2007 Aug; 293(2): E620–7
Aronne L, Fujioka K, Aroda V, et al. Progressive reduction in body weight after treatment with the amylin analog pramlintide in obese subjects: a phase 2, randomized, placebo-controlled, dose-escalation study. J Clin Endocrinol Metab 2007 Aug; 92(8): 2977–83
Amiel SA, Heller SR, MacDonald IA, et al. The effect of pramlintide on hormonal, metabolic, or symptomatic responses to insulin-induced hypoglycaemia in patients with type 1 diabetes. Diabetes Obes Metab 2005 Sep; 7(5): 504–16
Acknowledgments
Dr Steve Edelman is a consultant and stockholder of Amylin Pharmaceuticals, Inc., and has received honoraria for speaking engagements from Amylin Pharmaceuticals. Drs Holly Maier and Ken Wilhelm are employees and stockholders of Amylin Pharmaceuticals.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Edelman, S., Maier, H. & Wilhelm, K. Pramlintide in the Treatment of Diabetes Mellitus. BioDrugs 22, 375–386 (2008). https://doi.org/10.2165/0063030-200822060-00004
Published:
Issue Date:
DOI: https://doi.org/10.2165/0063030-200822060-00004